Combination of Bawang Dayak Extract and Acarbose against Male White Rat Glucose Levels
Abstract
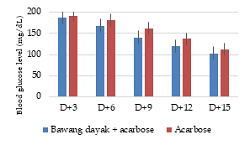
Diabetes is a chronic metabolic disease with signs of increased blood glucose levels. Type 2 diabetes is common diabetes in adults. Bawang dayak is one of the plants believed to have the efficacy of curing various types of diseases. The purpose of this study was to find out the comparison of hypoglycemic effects between combinations of bawang dayak extract and acarbose with single acarbose. This study was an experimental study using 32 white mice divided into two groups. Group one was given a combination of bawang dayak at a dose of 100 mg/kg BW and acarbose at a dose of 40 mg/100 g BW, while group two was given acarbose at a dose of 40 mg/100 g BW. Treatment is administered after the test animal is induced with dexamethasone at a 1 mg/kg BW dose dissolved in NaCl 0.9% subcutaneously for 12 days. Measurement of glucose levels was carried out using a glucometer. Data retrieval was carried out every three days for 15 days after previously fulfilled for +10 hours. Blood glucose level data were analyzed with the General Linear Model test. The combination of bawang dayak-acarbose onion extract had a greater decrease in blood glucose levels than single acarbose. Average reduction in blood glucose levels for D+3; D+6; D+9; D+12; and D+15 was 187.31; 168.56; 140.81; 119.81; and 102.56 mg/dl, respectively. The General Linear Model test results showed a p <0.05 value that significantly impacted blood glucose levels between groups.
Full text article
References
2. Vieira R, Souto SB, Sánchez-López E, Machado AL, Severino P, Jose S, et al. Sugar-Lowering Drugs for Type 2 Diabetes Mellitus and Metabolic Syndrome-Review of Classical and New Compounds: Part-I. Pharmaceuticals. 2019;12(4):152. doi:10.3390/ph12040152
3. Lin X, Xu Y, Pan X, Xu J, Ding Y, Sun X, et al. Global, regional, and national burden and trend of diabetes in 195 countries and territories: an analysis from 1990 to 2025. Sci Rep. 2020;10:14790. doi:10.1038/s41598-020-71908-9
4. Ligita T, Wicking K, Francis K, Harvey N, Nurjannah I. How people living with diabetes in Indonesia learn about their disease: A grounded theory study. PLoS One. 2019;14(2):e0212019. doi:10.1371/journal.pone.0212019
5. Skyler JS, Bakris GL, Bonifacio E, Darsow T, Eckel RH, Groop L, et al. Differentiation of Diabetes by Pathophysiology, Natural History, and Prognosis. Diabetes. 2017;66(2):241-55. doi:10.2337/db16-0806
6. Marín-Peñalver JJ, Martín-Timón I, Sevillano-Collantes C, del Cañizo-Gómez FJ. Update on the treatment of type 2 diabetes mellitus. World J Diabetes. 2016;7(17):354-95. doi:10.4239/wjd.v7.i17.354
7. Sami W, Ansari T, Butt NS, Hamid MRA. Effect of diet on type 2 diabetes mellitus: A review. Int J Health Sci. 2017;11(2):65-71.
8. Chaudhury A, Duvoor C, Dendi VSR, Kraleti S, Chada A, Ravilla R, et al. Clinical Review of Antidiabetic Drugs: Implications for Type 2 Diabetes Mellitus Management. Front Endocrinol. 2017;8:6. doi:10.3389/fendo.2017.00006
9. Chaturvedi R, Desai C, Patel P, Shah A, Dikshit RK. An evaluation of the impact of antidiabetic medication on treatment satisfaction and quality of life in patients of diabetes mellitus. Perspect Clin Res. 2018;9(1):15-22. doi:10.4103/picr.PICR_140_16
10. May M, Schindler C. Clinically and pharmacologically relevant interactions of antidiabetic drugs. Ther Adv Endocrinol Metab. 2016;7(2):69-83. doi:10.1177/2042018816638050
11. Choudhury H, Pandey M, Hua CK, Mun CS, Jing JK, Kong L, et al. An update on natural compounds in the remedy of diabetes mellitus: A systematic review. J Tradit Complement Med. 2018;8(3):361-76. doi:10.1016/j.jtcme.2017.08.012
12. Seca AML, Pinto DCGA. Biological Potential and Medical Use of Secondary Metabolites. Medicines. 2019;6(2):66. doi:10.3390/medicines6020066
13. Sofowora A, Ogunbodede E, Onayade A. The Role and Place of Medicinal Plants in the Strategies for Disease Prevention. Afr J Tradit Complement Altern Med. 2013;10(5):210-29. doi:10.4314/ajtcam.v10i5.2
14. Salehi B, Ata A, Kumar NVA, Sharopov F, Ramírez-Alarcón K, Ruiz-Ortega A, et al. Antidiabetic Potential of Medicinal Plants and Their Active Components. Biomolecules. 2019;9(10):551. doi:10.3390/biom9100551
15. Febrinda AE, Yuliana ND, Ridwan E, Wresdiyati T, Astawan M. Hyperglycemic control and diabetes complication preventive activities of bawang dayak (Eleutherine palmifolia L. Merr.) bulbs extracts in alloxan-diabetic rats. Int J Food Res. 2014;21(4):1405-11.
16. Wardani IGAAK, Megawati F, Suena NMDS. The Effect of Dayak Onion Bulb Ethanol Extract (Sisyrinchium palmifolium L.) on Triglyceride Level and Aorta Histopathology in Diabetes Melitus White Rat Induced by Alloxan. Majalah Obat Tradisional. 2019;24(2):77-84. doi:10.22146/mot.38051
17. Novaryatiin S, Ardhany SD. The antibacterial activity of bawang dayak (Eleutherine bulbosa (Mill.) Urb.) from central kalimantan against acne-causing bacteria. Int J Appl Pharm. 2019;11(5):22-5. doi:10.22159/ijap.2019.v11s5.T0032
18. Febrinda AE, Astawan M, Wresdiyati T, Yuliana ND. Kapasitas Antioksidan Dan Inhibitor Alfa Glukosidase Ekstrak Umbi Bawang Dayak [Antioxidant and Alpha-Glucosidase Inhibitory Properties of Bawang Dayak Bulb Extracts]. Jurnal Teknologi dan Industri Pangan. 2013;24(2):161-7. doi:10.6066/jtip.2013.24.2.161
19. Proenca C, Freitas M, Ribeiro D, Oliveira EFT, Sousa JLC, Tomé SM, et al. α-Glucosidase inhibition by flavonoids: an in vitro and in silico structure–activity relationship study. J Enzyme Inhib Med Chem. 2017;32(1):1216-28. doi:10.1080/14756366.2017.1368503
20. Yang HK, Lee SH, Shin J, Choi YH, Ahn YB, Lee BW, et al. Acarbose Add-on Therapy in Patients with Type 2 Diabetes Mellitus with Metformin and Sitagliptin Failure: A Multicenter, Randomized, Double-Blind, Placebo-Controlled Study. Diabetes Metab J. 2019;43(3):287-301. doi:10.4093/dmj.2018.0054
21. Zhang QW, Lin LG, Ye WC. Techniques for extraction and isolation of natural products: a comprehensive review. Chin Med. 2018;13:20. doi:10.1186/s13020-018-0177-x
22. Martínez BB, Pereira ACC, Muzetti JH, Telles FdP, Mundim FGL, Teixeira MA. Experimental model of glucocorticoid-induced insulin resistance. Acta Cir Bras. 2016;31(10):645-9. doi:10.1590/s0102-865020160100000001
23. Yuswi NCR. Ekstraksi Antioksidan Bawang Dayak (Eleutherine palmifolia) Dengan Metode Ultrasonic Bath (Kajian Jenis Pelarut Dan Lama Ekstraksi). Jurnal Pangan dan Agroindustri. 2017;5(1):71-9.
24. Novaryatiin S, Ramli A, Ardhany SD. Uji Daya Hambat Ekstrak Etanol Bawang Dayak (Eleutherine bulbosa (Mill.) Urb.) terhadap Bakteri Staphylococcus aureus. Jurnal Surya Medika (JSM). 2019;4(2):51-9. doi:10.33084/jsm.v4i2.565
25. King AJF. The use of animal models in diabetes research. Br J Pharmacol. 2012;166(3):877-94. doi:10.1111/j.1476-5381.2012.01911.x
26. Suh S, Park MK. Glucocorticoid-Induced Diabetes Mellitus: An Important but Overlooked Problem. Endocrinol Metab. 2017;32(2):180-9. doi:10.3803/EnM.2017.32.2.180
27. Morgan SA, Gathercole LL, Simonet C, Hassan-Smith ZK, Bujalska I, Guest P, et al. Regulation of lipid metabolism by glucocorticoids and 11β-HSD1 in skeletal muscle. Endocrinology. 2013;154(7):2374-84. doi:10.1210/en.2012-2214
28. Morgan SA, Sherlock M, Gathercole LL, Lavery GG, Lenaghan C, Bujalska IJ, et al. 11β-Hydroxysteroid Dehydrogenase Type 1 Regulates Glucocorticoid-Induced Insulin Resistance in Skeletal Muscle. Diabetes. 2009;58(11):2506-15. doi:10.2337/db09-0525
29. Kuo T, McQueen A, Chen TC, Wang JC. Regulation of Glucose Homeostasis by Glucocorticoids. Adv Exp Med Biol. 2015;872:99-126. doi:10.1007/978-1-4939-2895-8_5
30. Arwati N, Wirjatmadi B, Adriani M, Meilanani S, Winarni D, Hartiningsih S. The effect of dayak onion bulb-stem (Eleutherine palmifolia (l.,) Merr.) extract on blood glucose levels of mouse suffered diabetes mellitus. Health Notions. 2018;2(3):368-72.
31. Yaturramadhan H, Dalimunthe A, Widyawati T. The Effect of Ethanolic Extract of Dayak Onion (Eleutherine palmifolia (L) Merr) Tuber on Blood Glucose and Insulin Level of Streptozotocin-Induced Diabetic Wistar Rat. Asian J Pharm Res Dev. 2019;7(4):38-42. doi:10.22270/ajprd.v7i4.548
32. Al-Ishaq RK, Abotaleb M, Kubatka P, Kajo K, Büsselberg D. Flavonoids and Their Anti-Diabetic Effects: Cellular Mechanisms and Effects to Improve Blood Sugar Levels. Biomolecules. 2019;9(9):430. doi:10.3390/biom9090430
33. Zulcafli AS, Lim C, Ling AP, Chye S, Koh R. Antidiabetic Potential of Syzygium sp.: An Overview. Yale J Biol Med. 2020;93(2):307-25.
34. Oh YS. Plant-Derived Compounds Targeting Pancreatic Beta Cells for the Treatment of Diabetes. Evid Based Complement Alternat Med. 2015;2015:629863. doi:10.1155/2015/629863
Authors
Copyright (c) 2021 Aditya Maulana Perdana Putra, Ratih Pratiwi Sari, Siska Musiam

This work is licensed under a Creative Commons Attribution-ShareAlike 4.0 International License.
This work is licensed under a Creative Commons Attribution-ShareAlike 4.0 International License.
Authors continue to retain the copyright to the article if the article is published in the Borneo Journal of Pharmacy. They will also retain the publishing rights to the article without any restrictions.
Authors who publish in this journal agree to the following terms:
- Any article on the copyright is retained by the author(s).
- The author grants the journal the right of first publication with the work simultaneously licensed under a Creative Commons Attribution License that allows others to share work with an acknowledgment of the work authors and initial publications in this journal.
- Authors can enter into separate, additional contractual arrangements for the non-exclusive distribution of published articles (e.g., post-institutional repository) or publish them in a book, with acknowledgment of their initial publication in this journal.
- Authors are permitted and encouraged to post their work online (e.g., in institutional repositories or on their websites) prior to and during the submission process. This can lead to productive exchanges and earlier and greater citations of published work.
- The article and any associated published material are distributed under the Creative Commons Attribution-ShareAlike 4.0 International License.